
 Want to earn continuing education credit for this article? Learn more.
Want to earn continuing education credit for this article? Learn more.
While PAD describes cardiovascular disease’s impact on the extremities, it is likely a sign of widespread atherosclerosis. People with PAD face a six-to-seven times higher risk of heart attack or stroke. Early recognition and attention to this condition are important for stopping its progression, as therapy and lifestyle modifications can minimize the risk of hampered blood flow to the heart or brain.
In an effort to restore circulation to the extremities, it seems logical to administer massage to clients with PAD. However, these circumstances should be approached with caution. Because a client with peripheral arterial disease is more prone to deep vein thrombosis – physician communication, a careful approach to local massage, and education on this condition are imperative.
Signs and Symptoms
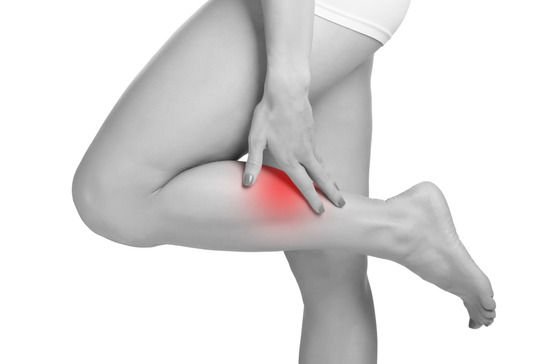
Approximately 50 percent of people with PAD have mild or no symptoms, while the other half develops more severe symptoms. Described as limb muscle pain or cramping triggered by activity and disappearing with rest, intermittent claudication is the most common symptom of PAD. While the calf is the most common location, the painful area depends on the location of the clogged or narrowed artery. Intermittent claudication can range from mild to debilitating, with the possibility of it prohibiting physical activity. Other signs and symptoms of peripheral arterial disease include:
- Leg numbness or weakness
- Cold legs or feet
- Non-healing sores on the toes, feet or legs
- A change in leg color
- Hair loss on the feet and legs
- Changes in the nails
If peripheral arterial disease progresses, pain may also occur during rest. Known as ischemic rest pain, this sensation may inhibit sleep. Ischemic rest pain may be temporarily relieved by hanging the legs over the edge of a bed or by walking around.
Risk Factors
Elements increasing the risk of developing peripheral arterial disease include:
- Smoking
- Being over age 50
- Diabetes
- Being overweight
- High blood pressure
- High cholesterol or high triglycerides
People who smoke or have diabetes have the greatest risk of complications from PAD; such as tissue death (gangrene) in a leg due to reduced blood flow. Early diagnosis and treatment of PAD is important not only to preserve limb health, but also to decrease risk of heart disease, stroke and other health problems.
Lifestyle Modifications
When caught early enough, the symptoms of PAD can be managed and its progression stopped. Stabilizing or improving peripheral arterial disease can be accomplished by the following lifestyle adjustments:
- Quitting Smoking – One of the most significant risk factors for PAD, smoking constricts and damages blood vessels.
- Exercising – Treating PAD is typically measured by how far a person can walk without leg pain. Exercise conditions muscles to use oxygen more efficiently. Many physicians rely on claudication exercise rehabilitation programs for management of PAD.
- Eating a Healthy Diet – Directly affecting the cardiovascular system, a heart-healthy diet can help control blood pressure and cholesterol levels. Avoiding foods high in saturated fat and cholesterol while choosing foods rich in omega-3 fatty acids (fatty cold-water fish, flaxseed, walnuts, soybeans and canola oil) can dramatically improve blood vessel health.
- Careful Foot Care – Taking good care of the feet is important for people with PAD and diabetes. This involves daily foot washing and moisturizing to prevent cracks, wearing well-fitting shoes and thick, dry socks, taking care when trimming toenails, avoiding walking barefoot, promptly treating foot fungal infections and seeing a doctor at the first sign of a foot sore or injury.
Massage Therapy
Using bodywork techniques on PAD can dramatically reduce a sufferer’s symptoms. However, care must be taken to avoid the loosening of a blood clot, which can have devastating consequences. We have assembled five suggestions from experts in the field of medical massage on working with the growing population of clients with peripheral arterial disease:
- Permission – This is not the time to be shy. If PAD is known, or even suspected, contact your client’s physician and get his/her permission prior to administering massage therapy. Dependant upon the client’s management of this disease, the physician may even offer tips on safely proceeding. Permission is especially important if the client demonstrates additional risk factors for deep vein thrombosis.
- Short Intervals – Benefits for PAD are most realized with massage sessions that are frequent yet of short duration. With affected legs, limit attention to the local area to two minutes per leg.
- Butterfly Tapotement – This technique created by Dietrich W. Miesler, MA, CMT is a gentle move aimed at loosening hardened muscle structures in the long muscles, especially the legs. It is executed with the client in the prone position, legs bent at the knees and resting against the chest of the therapist. By loosely drumming with the fingertips on the calf muscles, beginning at the ankles and slowly moving toward the popliteal area and repeating it several times, blood flow is increased.
- Fluffing – This hybrid move combines effleurage and petrissage. Another gentle technique, fluffing begins with gentle effleurage strokes towards the heart with the therapist stopping every inch for a relatively short squeeze. When following butterfly tapotement, the client’s position can remain the same. Fluffing must be done on a muscle in a relaxed position to receive the benefit of circulation enhancement. Fluffing is likely too strong for clients experiencing ischemic rest pain.
- Energy Work – A safe way to proceed with unknown cardiovascular status is administering energy work, such as Reiki or Therapeutic Touch. These techniques enhance local circulation without the mechanical force that could potentially cleave an arterial deposit.
Armed with the knowledge of peripheral arterial disease’s prevalence, symptoms and risk factors, massage therapists are at an advantage in working with these individuals. Understanding the lifestyle modifications and massage therapy techniques that can minimize PAD’s progression gives massage therapists the tools to confidently work with this disease. Because helping people return pain-free to their daily activities is an unbelievably rewarding feat, an increasing number of therapists are becoming educated on cardiovascular diseases and learning about the part they can play in circulatory health.
Earn continuing education credit for this article contained in our Common Pathologies & Complaints series. Click here to enroll.














Quite informative post it is. Thanks for sharing it.