
 Want to earn continuing education credit for this article? Learn more.
Want to earn continuing education credit for this article? Learn more.
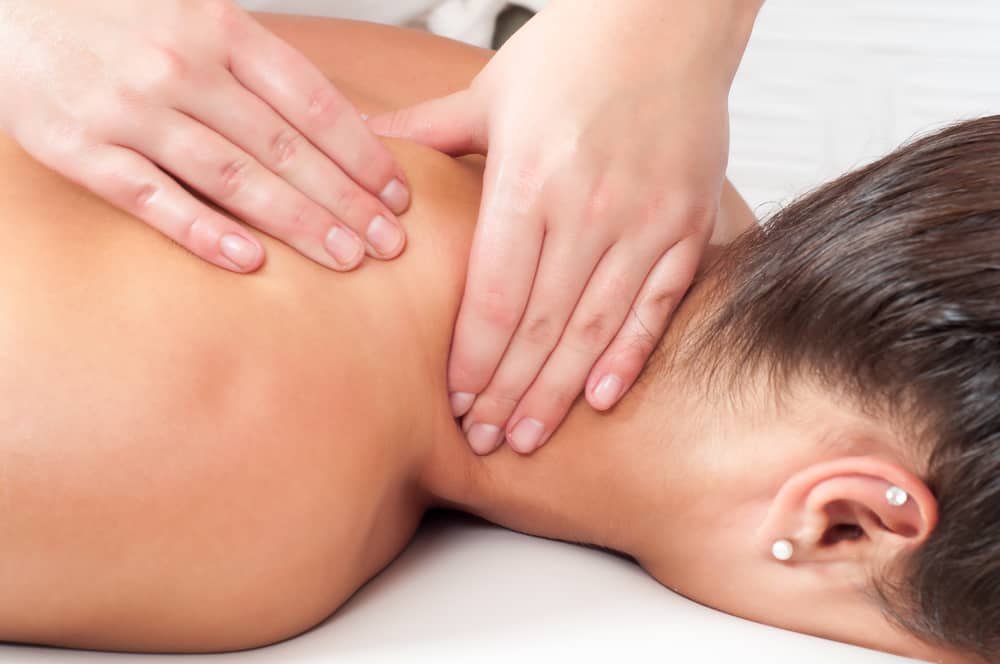
The chronic, widespread pain of fibromyalgia syndrome (FMS) typically manifests as stiffness and pain migrating throughout the body. Symptoms of FMS can include deep aching, burning, stabbing, or throbbing pain, draining fatigue, joint stiffness, and muscle weakness. While allopathic medicine has little to offer FMS sufferers, bodyworkers have the skills to address and relieve intense fascial and musculoskeletal pain manually.
Oxygenation
Due to the invigoration of blood and lymph circulation, massage facilitates tissue oxygenation, rendering it ideal for reducing stiffness and pain. A therapist may notice that an FMS client’s tender points are typically cold to the touch, indicating inhibition of circulation. Clinical research indicates that regular massage sessions normalize these temperature variations, and in doing so, reduce the severity of painful and stiff locations.
Flare-ups
Fibromyalgia recuperation does not progress linearly. Even a comprehensive pain management program will intermittently experience setbacks or flare-ups. The symptoms of a flare-up indicate oxygen insufficiency in the muscles and brain. Since massage increases tissue oxygenation, flare-ups present an ideal time to receive massage.
Bodyworkers must proceed carefully and slowly with FMS clients, especially when flare-ups are involved. During a flare-up, symptoms intensify, and new symptoms can develop. For some clients, vigorous strokes or deep pressure massage can cause rebound tenderness, exacerbating pain. Before and during flare-ups, certain areas may be too tender for deep work and can result in further tensing of the involved muscles. Respected fibromyalgia researcher, Devin J. Starlanyl, MD, recommends avoiding deep tissue massage or neuromuscular therapy during these times.
Signs of an impending flare-up include:
- Fasciculations – small twitches caused by groups of muscles that fire randomly. The jerks or spasms indicate that muscles or nerves are irritated. Before a flare-up, these twitches may worsen.
- Muscle strength can become unreliable. Those affected tend to drop things more frequently and lose coordination.
- Circulation may be impaired due to constricted blood vessels. One hand or foot may feel colder than the other.
- Memory and thinking may become impaired.
- Depression may worsen.
The right massage or energy technique can produce the relaxation and therapeutic results needed during a flare-up. During a flare-up’s onset or active phase, cranial-sacral or myofascial release may be the most effective therapy to restore musculoskeletal balance. Energy techniques can always be safely included in a massage to dissolve blockages, induce relaxation and harmonize the body.
In order to obtain a successful outcome with FMS, the massage technique must match your client’s immediate needs and preferences. Listed below are nine massage techniques that may greatly benefit someone with FMS:
- Myofascial Release is a technique developed by a physical therapist to gently relieve restrictions and tightness in connective tissue (fascia). When properly performed, it may decrease connective tissue’s pull on bones, allowing muscle fibers to relax and lengthen and organs to expand. Discoveries from six studies found that in both therapist- and self-administered sessions, this technique demonstrated an improvement in pain, sleep quality, and overall life satisfaction immediately after treatment. Yet, the improvements didn’t fade; its effects lingered even six months later, revealing the enduring impact of this therapy.
- Swedish Massage techniques are gentle but deep enough to reduce the pain associated with FMS effectively. One massage researcher, Richard Van Why, reported that Swedish vibration techniques, either administered by hand or mechanical means, powerfully relieved pain and caused the release of long-held tension in the muscles of those with FMS.
- Positional release techniques, frequently practiced by osteopathic physicians, are finding their way into massage therapy. The muscle energy technique (MET) and strain counter strain technique (SCS) are positional release techniques capable of normalizing dysfunctional neuromuscular relationships typical of FMS.
These techniques work with restriction barriers to improve local circulation, lengthen hypertonic tissue and restore range of motion. MET utilizes post-isometric relaxation and reciprocal inhibition to relax a muscular contraction and prepare the client for stretching or mobilizing a restricted joint. Ideal for clients with a high level of sensitivity, SCS involves shortening the tissue in acute spasms. - Reflexology is another suitable massage technique to address acute and chronic FMS conditions. Reflex areas on the feet and hands correspond with all of the areas and organs of the body. Gentle enough for all ages and conditions, this approach encourages the body to restore its healthy balance naturally.
- Passive stretching, alternatively called relaxed or static-passive stretching relieves muscle tension and spasms associated with FMS. A massage therapist can assist with this stretch by moving the limb or head to its restricted barrier, then maintaining the stretched position while the client fully relaxes. An appropriate passive stretch can increase the range of motion and help the loss of flexibility that typically develops with FMS. Empower your clients to reduce their own muscle fatigue and soreness by providing instructions on passive stretching exercises to perform at home.
- With passive stretching, proprioceptive neuromuscular facilitation (PNF) can stretch a muscle further. PNF involves the client pushing against the therapist’s resistance to allowing individual muscles and muscle groups to lengthen, reducing muscle hypertonicity.
- Energy healing is considered noninvasive, subtle, highly relaxing, and effective, prompting many FMS sufferers to seek energy healing practitioners. Energy techniques can promote tissue change without applying pressure on tender areas. While there are many energy techniques, two of the most highly respected and researched forms are Reiki and Therapeutic Touch.
- Cranial-Sacral Therapy (CST) resets and normalizes the rhythm of cerebrospinal fluid, bringing about physical adjustments to the myofascia. Emotional release often accompanies the release of myofasical tension, requiring active listening skills and a focused presence on the part of the therapist. Emotional releases are capable of reducing or eliminating physically-based chronic pain.
- Neuromuscular Therapy (NMT) is a specific and scientific approach to relieving muscular pain by balancing the musculoskeletal and nervous systems. As NMT involves working directly on trigger and tender points, accurate detection of FMS flare-ups and continual communication with FMS clients are crucial practitioner skills. When appropriate, this therapy can dramatically reduce pain and improve flexibility, balance, and strength by interrupting the transmission of pain and improving circulation in and around the affected musculature.
Effective fibromyalgia massage hinges on a bodyworker’s tactile sensitivity and ability to communicate and respond accordingly. While many bodyworkers value their intuition and minimize discussion during a session, this lack of verbal communication is inappropriate for FMS clients. Relying on a client to verbalize discomfort at the moment is accompanied by the risk of harming that client. Additionally, people with FMS may be skilled at masking their pain, so depending on your detection of a client’s discomfort may be unreliable.
A successful bodyworker must be proactive by constantly evaluating tissue quality for resistance to touch and verbally checking the client’s experience. When incorporated with sensitivity and communication, understanding the what, how, when, where and why of the massage applications listed above will benefit any FMS client in your care.
Editor’s Note: More information for massage therapists about fibromyalgia can be accessed in this series’ first article, Fibromyalgia Part 1: Fibromyalgia Relief with Massage.
Earn continuing education credit for this article contained in our The Impact of Fibromyalgia series. Click here to enroll.











